Gastroscopy
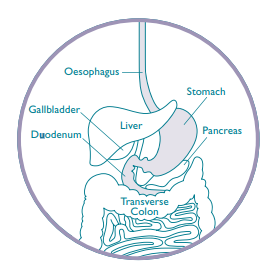
Gastroscopy is a visual examination of the lining of the oesophagus, stomach and duodenum (first part of your intestine). A flexible tube (about the thickness of a ball point pen) is passed through your mouth and into the stomach. The tube will not interfere with your breathing. A small video camera, which can take photos, sends an image onto a video screen. The doctor can look for any abnormalities and if necessary biopsies (small tissue samples) can be painlessly taken for laboratory testing. Other procedures to treat specific conditions can be done through the endoscope.
These include:
- Stretching (dilating) the narrowed areas of the oesophagus, stomach or duodenum.
- Removing polyps and swallowed objects.
- Treatment of bleeding vessels and ulcers by internal injection or diathermy.
You may be referred for a gastroscopy to investigate:
- Indigestion, heartburn, reflux
- Bleeding, anaemia
- Nausea
- Swallowing difficulties
- Pain or abdominal discomfort
|
During your procedure you will be given sedation. It is important that you arrange for someone to drive you home following your procedure. You are not permitted, by law, to drive yourself. For safety reasons, if you are travelling on public transport, or in a taxi, please arrange for a support person to travel with you.
|